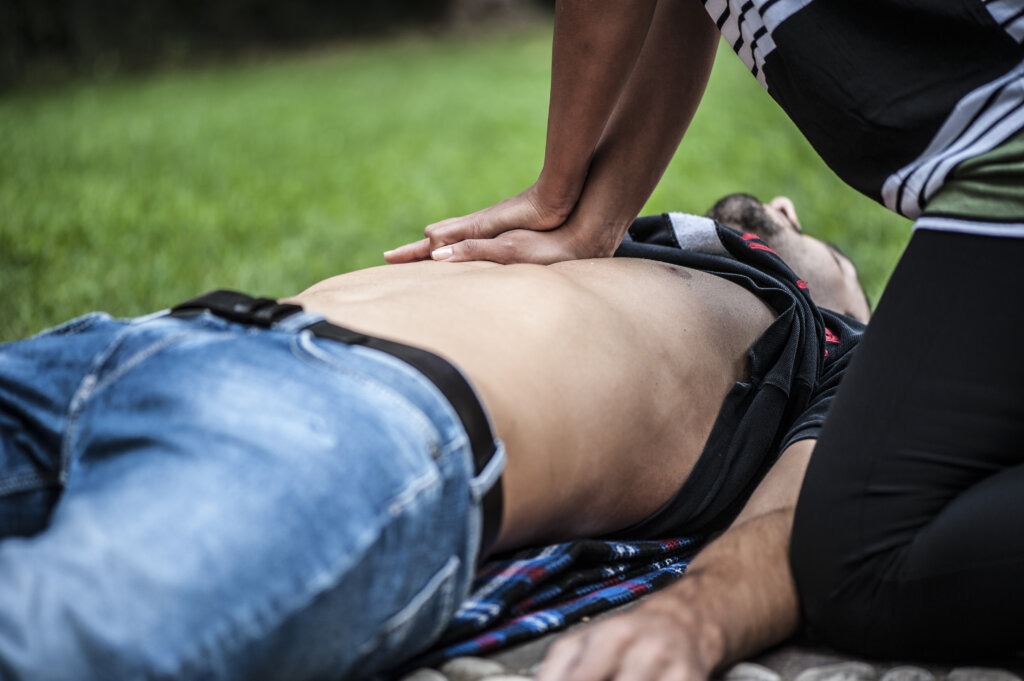
The 5 Components of High-Quality CPR – Metrics Beyond Rate and Depth
Compression rate and depth are the two metrics that dominate CPR training assessments, and for good reason — both have a direct relationship with survival outcomes. But focusing on them as the primary indicators of a quality resuscitation attempt creates a blind spot. Providers can compress at 110 per minute, hit five centimetres consistently, and still fail to generate the coronary perfusion pressure needed to achieve return of spontaneous circulation. The difference between a technically compliant attempt and a physiologically effective one is where survival is won or lost.
That gap exists because high-quality CPR is not defined by simply two variables. The AHA identifies five distinct performance components, each with its own physiological mechanism and its own consequence when neglected. Rate and depth are two of them. The other three — chest compression fraction, complete chest recoil, and controlled ventilation — are less visible, harder to self-monitor in real time, and more frequently compromised under the conditions of an actual resuscitation.
What High-Quality CPR Measures
The American Heart Association identifies five components that define high-quality CPR:
- Compression rate
- Compression depth
- Chest compression fraction (CCF)
- Full chest recoil
- Avoidance of excessive ventilation
Together, they serve a single physiological objective — generating and sustaining coronary perfusion pressure (CPP) high enough to maintain myocardial blood flow until either the heart restarts or advanced interventions take effect.
CPP is the pressure gradient between the aorta and the right atrium during the relaxation phase of each compression. It is the primary determinant of myocardial blood flow during cardiac arrest, and it is the variable that ultimately predicts whether ROSC is achievable. The challenge is that CPP cannot be measured directly at the bedside in most clinical settings. Providers instead rely on the five performance components as proxies — each one influences CPP through a specific mechanism, and a deficit in any one of them carries a real physiological cost.
This is why treating rate and depth as the headline metrics and the remaining three as supporting details is a category error. All five components interact. A compression delivered at the correct rate and depth but preceded by a five-second pause, or followed by incomplete recoil, or accompanied by over-ventilation, will generate less effective perfusion than one delivered within a well-controlled resuscitation that prioritises all five simultaneously.
Why Rate and Depth Only Tell Half the Story
A 2019 cohort study published in JAMA Network Open, drawing on NIH clinical trials registry data from 3,643 out-of-hospital cardiac arrest patients, identified the optimal compression rate-depth combination associated with functionally favourable survival as 107 compressions per minute at a depth of 4.7 centimetres. When CPR was performed within 20% of that combination, survival probability was significantly higher — an odds ratio of 1.44 compared to those outside the target range. That is a meaningful finding. It confirms that rate and depth matter, and that there is a measurable sweet spot worth aiming for. (Duval et al., 2019)
What the same data also makes clear is that hitting that combination does not guarantee survival, and that the benefit was most pronounced when a CPR adjunct device was in use — suggesting that the mechanical consistency of delivery matters as much as the numerical targets themselves.
There is also a practical execution problem. A study examining CPR quality among in-hospital providers found that while 56% of compressions fell within the target rate range and 39% within the target depth range, only 13.7% of compressions simultaneously met both targets. That figure reflects what real resuscitation looks like under clinical conditions, even with trained providers. Add the demands of airway management, rhythm interpretation, medication timing, and team coordination, and the margin for consistent mechanical execution narrows further. (Leo et al., 2023)
Chest Compression Fraction – The Metric That Gets Overlooked
Chest compression fraction is the proportion of total resuscitation time during which chest compressions are actively being delivered. It is calculated simply: cumulative compression time divided by total resuscitation time. The AHA target is a CCF of at least 80%, meaning that in a ten-minute resuscitation, compressions should be actively occurring for at least eight of those minutes. That target is harder to hit than it sounds.
Why Pauses Are So Costly
Every pause in compressions has an immediate physiological consequence. Coronary perfusion pressure builds gradually with sustained compressions and drops rapidly the moment they stop — it does not recover instantly when compressions resume. Animal model data has consistently demonstrated that even brief interruptions reduce both cerebral and coronary perfusion, and that it takes several compression cycles to rebuild the CPP lost during a hands-off interval. A pre-shock pause of just five to ten seconds is enough to meaningfully reduce the probability that defibrillation will succeed.
The Compounding Effect of Necessary Interruptions
Rhythm checks, defibrillation preparation, airway placement, and vascular access are all necessary components of resuscitation — but their cumulative effect on CCF is frequently underestimated. Each individually justified interruption compounds the others. A team that manages each pause efficiently may still end a resuscitation with a CCF well below 80% simply because the interruptions were frequent, even if each one was brief. Out-of-hospital cardiac arrest data consistently links lower CCF with decreased rates of ROSC and reduced survival, and that relationship becomes more pronounced the longer the resuscitation continues.
Why CCF Is Difficult to Self-Monitor
Without a feedback device, CCF is invisible in real time. A provider focused on compression quality has no internal clock tracking cumulative hands-off time. This is one of the strongest arguments for incorporating CPR feedback technology into resuscitation practice — and for ensuring that basic life support training addresses CCF not as a definition to memorise, but as a performance variable that requires deliberate team-level management.
Residual Leaning and Why It Compromises Recoil
Full chest recoil is the complete return of the chest wall to its natural position between compressions. It is the mechanism by which negative intrathoracic pressure is generated during CPR — that negative pressure draws venous blood back into the thorax and into the right side of the heart, replenishing the cardiac filling volume that the next compression will eject.
The Physiological Cost of Incomplete Recoil
When a provider’s hands remain in contact with the chest wall between compressions, even with modest residual force, that recoil is impaired. The consequences are direct and measurable:
- Intrathoracic pressure remains elevated between compressions
- Venous return to the right heart is reduced
- Cardiac filling volume ahead of the next compression is diminished
- The cardiac output generated by each subsequent compression is lower than it should be
Research published in Critical Care Medicine demonstrated that residual leaning during CPR impairs both cardiac output and left ventricular myocardial blood flow — confirming that incomplete recoil is not a minor technical deviation, but a meaningful reduction in resuscitation effectiveness.
Why Trained Providers Still Get This Wrong
Studies observing in-hospital CPR performance have found that leaning is common among trained providers, often occurring without their awareness. The physical demands of sustained compressions, combined with the need to maintain positioning over a patient on a bed or stretcher, create conditions where partial weight-bearing on the chest becomes the default rather than the exception.
Correcting residual leaning requires deliberate technique reinforcement during training, and ideally real-time feedback during resuscitation. It is one of the components of CPR quality that self-assessment cannot reliably detect — a provider cannot feel the difference between full recoil and 90% recoil while simultaneously managing compression rate, depth, and team communication. This is precisely the kind of deficit that structured basic life support training, with supervised skills assessment, is designed to identify and correct before it becomes an unexamined habit in clinical practice.
Ventilation – When Helping can be Harmful
Ventilation is the component of CPR most likely to be performed with good intent and poor outcome. The instinct to breathe for a patient in cardiac arrest is clinically sound — oxygen delivery matters. But the manner in which ventilation is delivered during resuscitation has a direct effect on the haemodynamic environment that compressions are working to maintain, and excessive ventilation is one of the most consistently documented performance failures in both pre- and in-hospital settings.
The Mechanism of Harm
Each positive pressure breath delivered during CPR increases intrathoracic pressure. When ventilation rate or tidal volume exceeds what is clinically appropriate, that pressure elevation becomes sustained rather than transient. The consequences follow the same physiological pathway as incomplete recoil:
- Venous return to the right heart is reduced
- Cardiac filling volume ahead of each compression is diminished
- Coronary perfusion pressure drops
- Cerebral perfusion is compromised
The 2025 AHA Guidelines for CPR and Emergency Cardiovascular Care reinforce controlled ventilation as a defined component of high-quality CPR precisely because the harm from over-ventilation is not theoretical — it is measurable and it is common.
What Controlled Ventilation Looks Like in Practice
For providers delivering CPR with a basic airway, the 30:2 compression-to-ventilation ratio exists to protect compression continuity while ensuring adequate oxygen delivery. Each breath should be delivered over approximately one second, producing visible chest rise without excessive force. Once an advanced airway is in place, ventilation shifts to a continuous rate of one breath every six seconds — ten breaths per minute — entirely asynchronous from compressions, which continue uninterrupted.
The most common deviation from this standard is stress-driven. Under the pressure of an active resuscitation, ventilation rate tends to increase and tidal volume tends to rise. Both move in the wrong direction. Awareness of this pattern, and the physiological reasoning behind controlled ventilation targets, is something that needs to be built during training rather than reasoned through in the middle of a resuscitation.
HSTCSA – Basic Life Support Training and Advanced Cardiovascular Life Support Course
High-quality CPR is not a single skill — it is a set of interdependent performance variables that must be understood, practised, and maintained to deliver consistent results under real clinical conditions. Rate and depth are the entry point. Chest compression fraction, complete recoil, and controlled ventilation are what separate a technically compliant attempt from one that generates the coronary perfusion pressure needed to give a patient a genuine chance at survival.
That level of performance requires training that builds physiological understanding alongside technical skill, and regular recertification that prevents the performance degradation that affects every provider over time, regardless of experience level.
At Health and Safety Training Centre of South Africa, we offer American Heart Association-aligned basic life support training and advanced cardiovascular life support courses designed for pre- and post-hospital healthcare professionals. Courses are structured to develop the individual technical competence and team-level coordination that high-quality resuscitation demands, with supervised skills assessment that identifies and corrects performance deficits before they become clinical habits.
If your BLS or ACLS certification is due for renewal, or if you are seeking provider qualification for the first time, enrolling with HSTCSA ensures your training reflects current evidence, current guidelines, and the standard of care your patients deserve.
References
Duval, S., Pepe, P.E., Aufderheide, T.P., et al. (2019) ‘Optimal combination of compression rate and depth during cardiopulmonary resuscitation for functionally favorable survival’, JAMA Cardiology, 4(9), pp. 900–908. doi:10.1001/jamacardio.2019.2717.
Leo, W.Z., Zhang, Z., Liu, N., et al. (2023) ‘Chest compression quality and patient outcomes with the use of a feedback device in in-hospital cardiac arrest’, Journal of Clinical Medicine, 12(20), Article 6573. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10645752/